I thought this was a good topic to talk about for now because there are so many people who have no idea what endometriosis and adenomyosis are. So I’m going to explain that here!
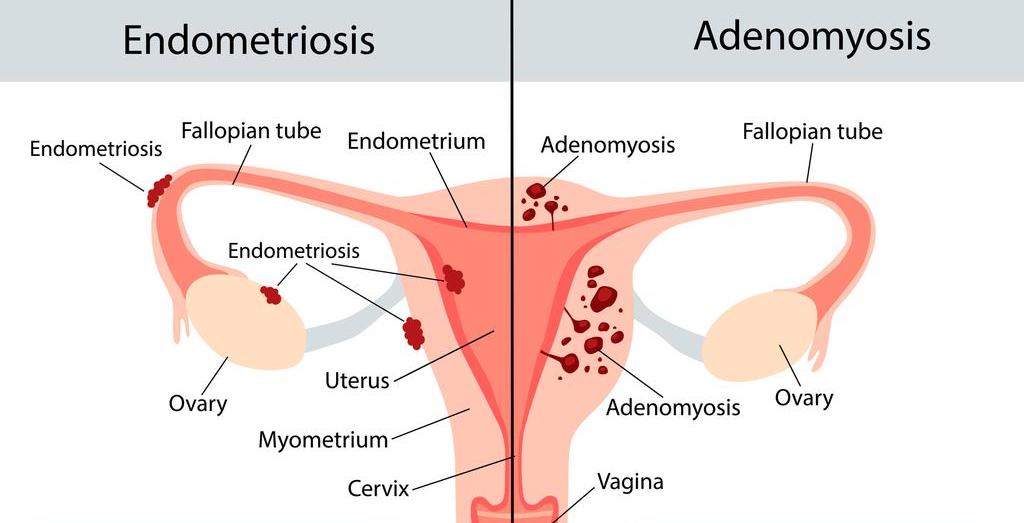
In endometriosis, tissue resembling the uterine lining (endometrium) outside the uterus grows.
This can be, for example, on the ovaries, fallopian tubes, peritoneum, intestines and/or bladder.

That tissue, like normal uterine mucosa, reacts to hormonal fluctuations during the menstrual cycle. It may swell and bleed, but the blood has nowhere to go. This often causes severe menstrual pain, chronic abdominal or pelvic pain, pain during sex, fatigue and/or fertility problems.
Endometriosis is a chronic condition and the symptoms vary greatly from person to person.
What is adenomyosis?
Adenomyosis is similar to endometriosis, but is located in a different place.
Here, uterine mucosa-like tissue grows in the muscle wall of the uterus (the myometrium).
As a result, the uterus is often enlarged, more sensitive and painful.
Common complaints are:
🩸Extremely painful periods
🩸very severe and/or prolonged blood loss
🩸a feeling of pressure or heavy in the lower abdomen
🩸Pain during sex
Adenomyosis is more common in people who have already given birth, but can also occur in others.
Important to know!
You can have both diseases at the same time.
The severity of pain says nothing about how extensive the condition is.
Complaints are still too often downplayed or recognized late.
Early recognition and good guidance really make a difference in quality of life.
Now you may be wondering: what is the cause of these diseases? I asked myself that and answered it below.
The short, honest answer is: the exact cause is not (yet) known. However, there are clear theories and risk factors.
I list them clearly and understandably for you, and I distinguish between endometriosis, adenomyosis and what they have in common.
Possible causes of endometriosis:
Retrograde menstruation
This is the most famous theory. During menstruation, part of the blood flows back into the abdominal cavity through the fallopian tubes. That blood contains cells from the uterine mucosa, which can settle there and continue to grow.
☝🏼 Many people have retrograde menstruation, but not everyone develops endometriosis, so this is probably not the only explanation.
Problems with the immune system
Normally, the immune system cleans up cells that are in the wrong place. In endometriosis, this system seems to work less well, allowing these cells to survive and cause inflammation.
Hormonal factors
Endometriosis is estrogen-sensitive. Higher exposure to estrogen (for example, due to early first menstruation or short cycles) may increase the risk.
Hereditary predisposition
Endometriosis is more common in families. If a mother, sister or aunt has it, you are more likely to develop it as well.
Metaplasia (cell change)
According to this theory, certain abdominal cells can transform themselves into uterine-like tissue, under the influence of hormones or inflammation.
Possible causes of adenomyosis:
Adenomyosis is less well researched, but these explanations are most often mentioned:
Ingrowth of the uterine mucosa:
The uterine mucosa grows from the inside into the muscle wall. This can happen after deliveries, a caesarean section, curettage or other uterine operations. Curettage is a medical procedure in which the doctor empties the inside of the uterus. This is done by removing the uterine mucosa (and any remaining tissue).
Disrupted border layer
There is normally a clear separation layer between the mucous membrane and the muscle wall. In adenomyosis, this barrier appears to be damaged or disrupted.
Hormonal influence
Adenomyosis is also highly dependent on estrogen, which can strengthen growth and complaints.
Endometriosis and adenomyosis share many risk factors:
🩸Early first menstruation
🩸Short menstrual cycles
🩸heavy or prolonged periods
🩸Long-term estrogen exposure
🩸Genetic predisposition
🩸Chronic inflammatory reactions
What we know for sure (and what we don’t)
❌ It’s not a mental health problem
❌ It is not due to “initiation” or low pain threshold
❌ It is not caused by stress, although stress can worsen symptoms
✅ They are real, physical diseases
✅ They can start as early as the teenage years
But then… how can we solve this? I have searched and below are treatments for endometriosis and adenomyosis.
Starting with the typical pyrelic such as paracetamol and ibuprofen and the like.
Because both conditions are sensitive to estrogen, attempts are often made to suppress the cycle.
Commonly used options:
🩸Contraceptive pill (often without a stop week)
🩸Progestogen (tablet, pill or hormone spiral)
🩸Hormone spiral (Mirena) – especially effective in adenomyosis
🩸GnRH agonists or antagonists
→ temporarily put the body into a kind of artificial transition.
Advantages:
Less pain.
Less or no menstruation.
Disadvantages:
side effects (mood complaints, fatigue, hot flashes).
Doesn’t work for everyone.
Complaints may come back after stopping.
Then there is the possibility of an operation. In endometriosis, this is Laparoscopy. This is a vision operation in which endometiosis fires are removed or burned away.
That can reduce pain and improve fertility, but endometriosis can come back.
Because addenomyosis is in the uterine wall, this is more difficult to operate on. There are possibilities for this:
🩸Hormone spiral
🩸Uterine-saving treatments (in specific cases)
removal of the uterus (hysterectomy) This is the only definitive solution for adenomyosis.
There are other treatments around fertility in case the woman wants to have children. This is all custom work.
Last but not least, you have additional and supportive care. These do not cure the condition but can help with complaints. These are :
🩸Pelvic physiotherapy
🩸Pain rehabilitation
🩸Dietary adjustments (e.g. anti-inflammatory diet)
🩸Psychological support
🩸Contact with fellow sufferers
The plague is, what works for one person does not have to work for the other… each person is of course unique and the right treatment is often searching and adjusting.
And what doctors see as “bearable” pain can also be terribly life-disrupting. That’s a perfect word for it.
Of course, it also plays a role in whether the woman wants to have children or not.
In my case, I don’t have it. I want my uterus out as soon as possible. Of course, there are also possible consequences, and I will briefly mention them.
👍🏼No more periods
👍🏼Pregnancy is no longer possible (definitively)
👍🏼Pain symptoms due to adenomyosis often disappear, but:
In endometriosis, symptoms can persist if there is also endometriosis outside the uterus.
👍🏼Hormones usually stay the same
→ Provided the ovaries are preserved
If the ovaries are also removed, immediate transition occurs.
👍🏼Recovery time
Physical recovery takes weeks to months.
Fatigue can last for a long time.
👍🏼Effect on sexuality
For some, less pain and more relaxation.
For others, change in feeling or experience.
👍🏼Emotional impact
👍🏼Relief from pain reduction
But also mourning, grief or identity questions (especially in the case of unfulfilled desire to have children).

❗️Important to emphasize❗️
A hysterectomy is irreversible.
It is not a light or quick fix.
Good information and informed choice are essential.
It is often a last treatment option for severe adenomyosis.
Thank you for reading and if you want to follow my personal journey, you can do so both on Instagram and here on my blog about my period. 🩷